The Human Development Report Office (HDRO) of the United Nations Development Programme (UNDP) has recently published a statistical analysis of the preparedness of the countries for responding to the COVID-19 pandemic and has pointed out the most vulnerable population groups.
The analysis referred to above is not an epidemiological one, it is not even an analysis of the public health situation in the world; it is an analysis of the level of preparedness of societies (or countries) to respond to a crisis of this type and intensity. It is clear that the COVID-19 pandemic crisis is more than a global public health threat; it is a systemic crisis of human development, which reflects our disrupted interaction with nature and its ecosystems, the insupportable inequalities among people and unsustainable economic activities.
This analysis confirms that there is a need for an adequate human development policy, both in the short and in the long term, which should include measures for reducing vulnerability and increasing resilience to shocks and crises, and points to the need for a continual development of capacities for resolving crises. Such measures are of vital importance for enabling individuals and society to protect themselves from these shocks and to recover from them fast.
The original analysis contains two data dashboards which present selected indicators that enable a quick visual estimate of the preparedness of the given country to respond to a crisis like the COVID-19 pandemic, and they also provide an analysis of particularly vulnerable population groups.
The countries with a high level of human development, that is, those whose citizens have a longer life expectancy, a higher quality and level of average education, a higher living standard, the states with a lower level of inequality, a better social care system, free from poverty and with a diverse economy, with a quality state administration, with advanced state and social institutions, are generally better positioned to respond to shocks and are capable of recovering from crises faster.
The public health crisis
We can quite rightly say that no state in the world was sufficiently prepared to deal with a pandemic caused by a new and unknown virus of this level of intensity, even though it is possible to observe differences in the level of development of health care systems through an analysis of the existing hospital capacities and the number of experts specialised for providing medical help and treating the sick.
Our analysis of the level of preparedness of a health care system took into consideration only four indicators – the number of doctors, the number of nurses and the number of hospital beds per 10,000 people, as well as the percentage of the gross domestic product (BDP) allocated for health care.
There exist great differences when one compares these indicators in developed and developing countries. For example, countries in the very high human development category have, on average, 30 doctors, 81 nurses and 55 hospital beds per 10,000 people, whereas the least developed countries have 2.5 doctors, 6 nurses and 7 hospital beds per 10,000 inhabitants. Unfortunately, these are the least developed countries in the world, mostly located in Africa below the Sahara. In these countries other contagious diseases also claim millions of lives each year. According to the World Health Organization (WHO) data, in the year 2016 over 3 million deaths were ascribed to respiratory infections, 1.4 million deaths to infection-related diarrhoea, 1.3 million people died of tuberculosis, one million people died of AIDS and around half a million people died of malaria. In these countries, the focus is on eradicating poverty and hunger, on improving the standard of living, on clean drinking water, on safe sanitary equipment and, certainly, on adequate medical treatment by means of vaccines and medicines. But the socio-economic aspect of these illnesses must not be neglected, for it is often more important than the medical one.
Differences in the values of these indicators also exist between developed European countries. The diagram below provides the minimum and maximum values of these indicators in the European Union (including Great Britain).
Source: The United Nations Development Programme (2020), http://hdr.undp.org
Differences also exist in our immediate surroundings, among the countries of the Western Balkans. Serbia has more doctors and hospital beds compared to the neighbouring countries, a negligibly lower percentage of health care expenditure than Bosnia and Herzegovina, but in terms of the number of nurses, it is considerably behind Croatia.
Source: The United Nations Development Programme (2020), http://hdr.undp.org
It is often observed that the spread of the coronavirus epidemic has hit hardest the countries with developed health care systems such as Great Britain, Italy, Belgium. However, the spread of the coronavirus, in terms of the number of people contaminated over a given period of time, is least dependent on the level of development of the given country’s health care system. The spread of the virus depends on a multitude of factors that are not necessarily related to health care – population density, dependence on public transportation, the period of time required for travelling to work, public gatherings, to name but a few. The level of success of measures undertaken for the purpose of suppressing the spread of the virus – personal hygiene (washing one’s hands), social distancing, quarantine, depend on the dimensions of human development referred to above – the level of education, equality, the standard of living of the population, solidarity, cohesion, Internet access and, to a large degree, on the quality of state and social institutions and the level of citizens’ trust in them.
The capacity of the given health care system becomes an important factor when it comes to the treatment of those infected – whether all those who suspect that they have been infected or are manifesting the symptoms can count on being subjected to an adequate diagnostic test and provided with medical attention, treatment and care.
The majority of countries plan their health care capacities on the basis of the estimated average needs. For example, hospital capacities are rarely engaged at a level exceeding 70 per cent. Epidemics are an exception to this general rule. On account of the COVID-19 pandemic, many countries have had to open new hospitals, often enough of an improvised nature, in order to be able to organise the treatment and care of the infected. That is why it was important to slow down the spread of the epidemic and to postpone the arrival of its shock wave.
The coronavirus has surprised the world due to its contagiousness, and in most countries it took time to make an adequate assessment of the magnitude of the problem. A part of this is certainly the provision of personal protection means such as masks or medical gloves, a sufficient number of medical devices such as respirators and special ventilators. How well a country is supplied with those depends on the flexibility of its industry and commerce rather than on the state of development of its health care system. The political leadership and the structure of decision-making also play a part in this crisis. That part is what defines the quality of the state administration and institutions.
The importance of the communications technology
The broad implementation of isolation and social distancing have led to a situation in which many had to rely on Internet access from home in order to continue working or attending school, and also to maintain communication with others. The digital divide has become more important that ever before, for several billion people in the world over still lack access to reliable broadband internet from home. Internet access has become a basic need. Uneven broadband internet access and the digital divide are also indicators of inequality in a society.
We must not neglect the role and importance of mobile phones for maintaining connections at the time of the COVID-19 pandemic in an interlinked world: contact with family and friends, contact with medical professionals – telehealth, medical consultations. Also, some forms of business can be conducted over the phone, ordering or offering and selling goods. But perhaps the most important thing of all is that mobile phones enable people to receive information on the virus, its local spread, infected personal contacts. A good example of this is the use of mobile phones to successfully suppress the spread of the coronavirus in South Korea.
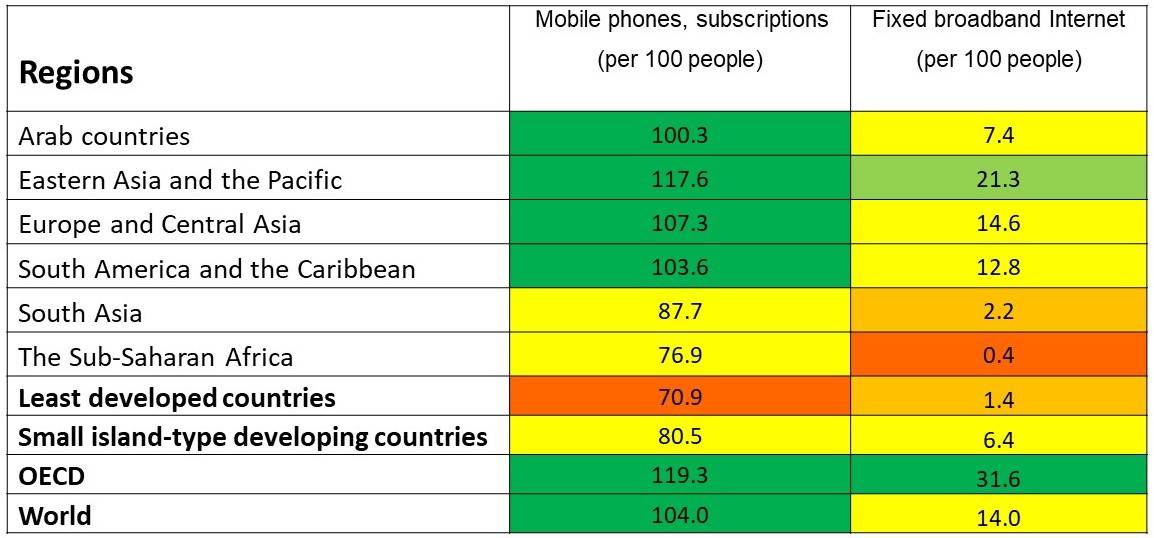
The table below shows the number of mobile phones and broadband internet connections per 100 people in UN development regions in 2018.
Source: The United Nations Development Programme (2020), http://hdr.undp.org Note: It is possible to have several phones registered to one and the same person – private, business, lost, uncancelled.
Increased risk groups
Even though everyone is potentially affected by this pandemic in one way or another, some individuals and groups are more vulnerable than others, sustain much greater damage and take a lot more time to recover. The original analysis shows the percentage of the population subject to multidimensional poverty, without any social protection, as well as the degree of dependence of national economies on remittances from abroad, official subventions for development and tourism.
Our estimate is that there are around 1.3 billion people in the world living in poverty, deprived of many aspects of life that the majority of people have reason to value and take for granted, such as the possibility for school-age children to attend school, to be sufficiently well fed not to lag in physical and mental development, to have access to clean drinking water, safe sanitary equipment, not to use solid fuel for cooking or heating, to have electricity, etc. An additional 900 million people are on the verge of becoming poor if they are exposed to a health, economic or climate shock or crisis. This means that more than a quarter of mankind lives in multidimensional poverty or is on the verge of becoming poor. The population segment living in multidimensional poverty is faced with a greater risk from the pandemic and from the economic crisis that occurs as its consequence.
Our data show that more than 40 percent of the world population have no social protection – no health care, no unemployment benefits, no unpaid maternity leave, no paid sickness leave, no paid annual holidays, no old age retirement.
Globalisation has brought new possibilities and increased efficiency, but we are witnessing how, on account of the COVID-19 pandemic, disruptions occurring in one place within the framework of an economy can cause grave local problems in other places. The effects of such events can be harmful for people who, for instance, greatly depend on tourism, such as island countries, on remittances from abroad or on receiving official financial assistance for the purpose of development.
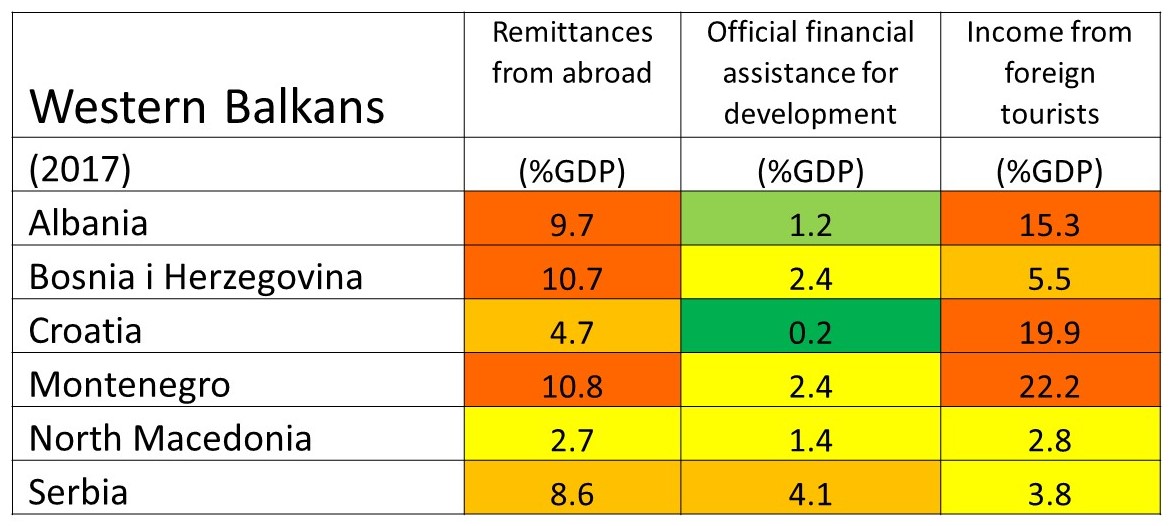
The table below shows that the economies of Western Balkans countries are dependent on the forms of revenues coming from abroad referred to above.
Source: The United Nations Development Programme (2020), http://hdr.undp.org
A return to normalcy?
To paraphrase a street graffiti from Hong Kong: “There is no return to ‘normal’, for ‘normal’ was the problem in the first place.”
The pandemic is a systemic crisis of human development that influences the economic and social aspects of development in ways that were impossible to predict. However, the fact that we are all exposed to danger should unite us, and through compassion, solidarity and creativity we should come out of this stronger, more resilient and humane. It is difficult to envisage how the world economies and life will change, but it is time for changes. Starting from extreme inequalities, insupportable exploitation of nature and degradation of the soil, water and air, to climate change that is increasingly intense – which are changing ecosystems and bringing tropical conditions to regions that were subtropical until recently. The warmer, more humid and changeable weather conditions are dependable signs of climate change that facilitates the spread of diseases to which we are not immune. There is still hope that, by resolving the current crisis, we shall begin to resolve the long-postponed problem of climate change and extreme inequality.
The blog was originally published as an op-ed in Novi magazin, issue 472.

 Locations
Locations