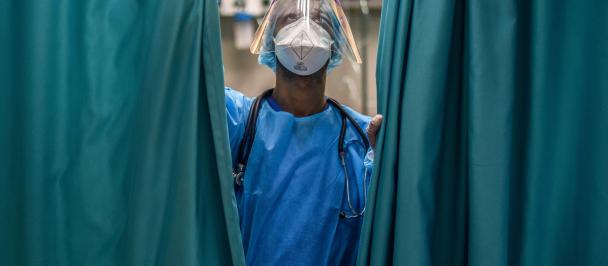
Without government stimulus programmes, hundreds of millions of people will lose their livelihoods during the coronavirus pandemic.
Temporary basic income and universal healthcare are both necessary to support people through this time.
They are already working in some countries.
With more than 55 million cases of COVID-19 reported at time of writing, many countries are struggling with second waves of the virus. The prospect of re-imposing lockdowns and other restrictions, while necessary to bring the pandemic under control, could have devastating economic and social consequences for millions. At the same time, many initial government stimulus plans that provide emergency cash assistance to the most vulnerable are coming to an end.
Without these programmes, hundreds of millions who lost their jobs or are struggling to make ends meet amid the pandemic must make difficult choices about how to use their limited resources. For many, the choice between spending money on medical expenses or necessities like food and shelter is, quite literally, life or death. Even if such social and economic protections continue, the lack of widely accessible and affordable health services means one medical bill could still force a family into extreme poverty.
Policymakers must use a combination of tools, including immediate measures such as temporary basic income and urgent changes like achieving universal health coverage, in their response. Only then can we recover from the pandemic and build back more resilient and sustainable communities.
Several countries have already implemented successful programmes to mitigate the financial impact of the COVID-19 pandemic. A recent UNDP report affirms that temporary basic income policies can help protect poor families that lack social assistance or insurance protection from the worst effects of the crisis.
The Colombian government has introduced the 'Solidarity Income' scheme to deliver resources to an additional three million vulnerable households. Meanwhile, the government of Togo gave over US$19.5 million in monthly digital cash transfers to more than 12 percent of its population, mostly women who work in the informal sector.
But temporary financial assistance is not enough. Without affordable healthcare, these types of programmes will inevitably fail to stimulate the economy and prevent financial hardship for the poorest and most vulnerable. United Nations Secretary-General António Guterres underscored this reality in his recent call for countries to urgently scale up investment in universal health coverage. As he put it: “A huge gap in health coverage is one reason why COVID-19 has caused so much pain and suffering.”
Women comprise 89 percent of the informal economy in sub-Saharan Africa. These informal workers, such as street vendors or domestic workers who have no social protection, could face enormous financial burdens due to health costs that would erase any economic gains from temporary basic income programmes. Even before the pandemic, 100 million people were pushed into extreme poverty each year because of healthcare costs. COVID-19 has only exacerbated this crisis, with disproportionate impacts on women and other marginalized groups.
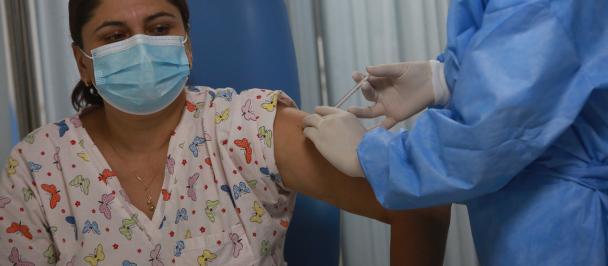
Despite income assistance, informal workers might forgo COVID-19 testing and unknowingly contribute to the spread of the pandemic due to the lack of affordable and accessible health services in many communities. Moreover, the stress of COVID-19 is disrupting other life-saving health services in these communities, such as childhood immunization, HIV, TB, malaria, maternal health care, family planning and treatment for noncommunicable diseases like diabetes and high blood pressure. These ripple effects multiply and could have harmful long-term effects for individuals, communities and national economies.
No one should be forced to choose between their health and their financial security. Investing in Temporary Basic Income (TBI) programmes and Universal Health Coverage (UHC) is the best strategy for long-term recovery by ensuring that people can get health care without facing serious financial difficulties. And it is possible to do both.
UNDP found that the majority of TBI schemes would cost most developing countries far less than one percent of their GDP per month, while providing substantial benefits to vulnerable families who need assistance to buy immediate necessities like food for their families.
While countries have agreed to work to implementing UHC by 2030, we must accelerate this process. For these precise reasons, Secretary-General Guterres has outlined how investing in UHC will help countries more effectively address the virus and its disruption of essential health services and its socioeconomic impacts, while contributing to long-term societal and economic resilience.
Studies show that UHC is an ambitious but attainable goal, even for the world’s poorest countries. Equitable affordable, high-quality healthcare is the foundation of resilient health systems that can respond in future emergencies and deliver essential services in times of both crisis and calm.
Temporary basic income can mitigate some of the worst effects of COVID-19 on poor households, and UHC is critical to ensuring strong health systems that don’t drive people into poverty, now or in the future. Both will take political will and investment, but now is not the time to limit or pull back. To respond effectively to COVID-19, countries should implement a smart combination of measures that will accelerate economic recovery while providing the foundation for more equitable, just and sustainable development. Only then can we protect the most vulnerable during this pandemic and prevent future health and economic crises.

 Locations
Locations